Proton therapy: looking for the ‘how?’
This year, the MAASTRO clinic in Maastricht is starting to use proton therapy—the promising new form of radiation treatment for cancer. The ‘what and why’ are no longer in question. Irradiation with protons instead of with photons can make a big difference for some types of cancer. The biggest question now revolves around the ‘how’: How can the therapy be best applied, in combination with other treatments, among other things? What is the optimal dosage? These and other questions will be answered by researchers from Maastricht University and MAASTRO clinic, in collaboration with colleagues from four other universities. The consortium has received a € 1.7 million grant for this from the Dutch Cancer Society (KWF).
The project, led by Prof. Rob Coppes of the UMC Groningen, is divided into three sub-projects. Because of its expertise, Maastricht is focusing primarily on package two. Marc Vooijs is a professor of Radiation Oncology. He heads the laboratory research within the Radiotherapy department of MUMC+ and Maastro Clinic and was co-applicant of the KWF grant.
Organoids for testing combinations
“Here, we have developed a way to grow in the laboratory the most aggressive cancer cells directly from patients, which we call ‘organoids’. This way, you can research how a patient will respond to a treatment. You can analyse both the healthy tissue and the tumour in that respect. Using this method, we expect to find, for example, the best combinations of proton therapy with immunotherapy relatively quickly, so that we can start patient studies as soon as possible.” To make optimal use of each other’s expertise, the organoids cultured in Maastricht go to the Erasmus University in Rotterdam, where they have expertise in the repair of DNA after radiation-induced damage.
In addition to studies on cell models, the consortium will also work with laboratory animals. “The effects of radiation on cognitive function (i.e. how information is recorded and processed by the brain) can’t be researched in just cells”, explains Vooijs. Amongst other things, these insights are of vital importance for children with brain cancer who are exposed to radiation, not only in the tumour cells, but also in some of their healthy brain cells.
The ratio behind the radiation dosage
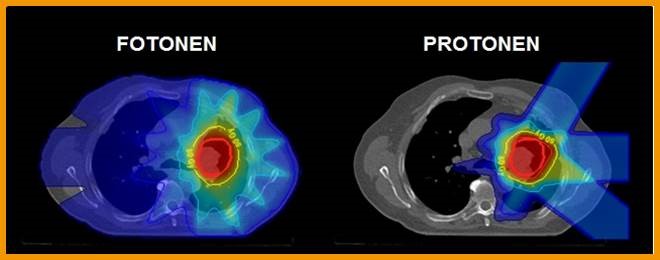
One of the big research questions involves the ‘therapeutic ratio’ for proton therapy, i.e. the highest possible dosage for a tumour with the least serious side effects for the patient. Which does not mean that it is an experimental treatment, says Dirk De Ruysscher, professor of Radiotherapy and Radiotherapist-Oncologist in Maastricht. He not only treats patients, but also conducts research into proton radiation. “We still think we can achieve a lot of benefits for the patient with proton therapy, especially in combination with immunotherapy. The traditional form of photon radiation involves a lot of ‘stray radiation’ on healthy tissue (blue in the image below). This doesn’t occur nearly as much with protons and that means fewer side effects for the patient.” The doctor explains that damaged tissue always wants to repair itself and certain proteins are produced for that. Unfortunately, the same proteins also fuel the growth of cancer cells. “We hope to be able to break this vicious cycle if there is less of that ‘scattered radiation’. If we succeed, we have an additional way to suppress cancer growth.”
What the future brings: avatars and multicentre studies
Prof. De Ruysscher is already working on a grant application to submit later this year, so that a ‘multicentre study’ on the effectiveness of proton therapy can begin. The four centres where proton therapy takes place can then combine their results, which will lead to a more sound knowledge base. Prof. Vooijs expects that organoid technology can also be used for the treatment of people with cancer in the near future. “In the laboratory, we can make copies of the tumour and of healthy tissue from that patient, so-called avatars. Then you can test the many combinations of treatment options on these avatars, so that you’ll know much more quickly which treatment is most effective for this patient.” Patients then no longer have to undergo treatments that have already been shown beforehand to be ineffective; they will only receive those treatments where the chance of success is greatest. “With this organoid expertise and the strong translational research and multidisciplinary collaborations in oncology within MUMC+, this is a huge opportunity for Maastricht to become a forerunner worldwide”, says Vooijs.
Also read
-
Stool samples as a key to health
Brightlands Campus Greenport Venlo is welcoming a new company this fall: InnerBuddies. This first Maastricht University spin-off is setting up shop at the campus with 27-year-old Jella Theeuwen at the helm as CEO.