“People finding each other is crucial for innovation”
Tim Welting and Paul Willems were both appointed professors in 2020. Quietly, as they have not yet been able to celebrate their inaugurations. After all, you can’t throw a party during a pandemic. But what you can do is give an online interview. Here, they talk about their work, their plans, and what drives them.
Both new professors work in the department of Orthopaedic Surgery at the Maastricht University Medical Centre (MUMC+) and are connected to CAPHRI's research line Functioning, Participation and Rehabilitation. Paul Willems is a professor of Integrated Spinal Care, an orthopaedic surgeon and the project leader of Spine Centre Maastricht. Tim Welting is a professor of Experimental Orthopaedics specialised in molecular cartilage biology. As head of the Laboratory for Experimental Orthopaedics, he spends most of his time in the lab. Even so, Willems and Welting see each other regularly – usually, that is. “That’s the great thing about my work”, says Welting. “The laboratory is very directly involved in clinical questions. I study the molecular biology of growing, healthy, diseased and aged cartilage. Disruption of molecular biological processes within cartilage play a major role in the development of osteoarthritis, a common and painful joint disease. Currently, the standard course of treatment only treats the symptoms of osteoarthritis: we replace a hip or focus on pain management. But if we learn more about the molecular basis of osteoarthritis, we may find ways to treat it at the source. We are also investigating when it’s better to take the traditional orthopedic approach (hip or knee replacement surgery) and when a biomolecular treatment is a better option for the patient”.
Osteoarthritis drug
And Welting is onto something. “A few years ago, we discovered together with our laboratory team that a naturally occurring growth factor (protein) in the human body – called BMP7 – has a very positive effect on osteoarthritic cartilage cells. We managed to replicate tiny pieces of proteins (peptides) of this BMP7 growth factor. In the lab, these peptides turned out to be successful in slowing down the progression of osteoarthritis. If these positive results occur in the human body as well, we will be one step closer to developing a drug for osteoarthritis. The patent for this discovery is held by our start-up company at Brightlands Maastricht Health Campus, Chondropeptix. We hope that the results of our fundamental cartilage research will lead to the discovery of even more molecules like these in order to treat osteoarthritis in various biomolecular ways.
From the molecular to the societal level
Welting may be conducting research at the molecular level, but he is looking to solve a serious problem in society at large. Almost 1.5 million people in the Netherlands suffer from osteoarthritis. “Our population is getting older and the number of patients with debilitating arthritis continues to increase. Part of our musculoskeletal system was not built for getting that old at all. I want to find smart molecular solutions to this problem.”

Tim Welting, PhD.
Professor of Experimental Orthopaedics, in particular molecular cartilage biology.
Picture: Appie Derks
The best care for each individual patient
Welting’s colleague Paul Willems is also looking for smart solutions. And he doesn’t necessarily need to find them within the walls of the university hospital. Providing “the right care in the right place” was the purpose he had in mind when he established Stadspoli Rug, an outpatient clinic focused on back problems. “Patients with neck and back problems used to be automatically referred to the hospital. But after proper medical examination, most patients can be treated by primary care providers like a physiotherapist and/or their general practitioner. The back clinic provides health care at the interface between primary and secondary care. Here, MUMC+ specialists hold out-of-hospital consultation hours for patients who were referred by their GP. Orthopaedic surgeons, neurologists and anaesthesiologists work together in a uniform, standardised way to diagnose the cause of the symptoms and refer the patient to the right care provider. This way, patients have faster access to the right treatment plan and we manage to keep the majority of these patients from needing hospital care, which is more expensive. A small number of patients are referred for further specialist examination or treatment.”
Treatment as well as support
They also collect as much patient data as possible in the back clinic and clinical settings. “This will give us an idea of which treatment works best for which type of patient and how high the risk of complications is. It allows us to predict the treatment outcome more accurately and talk about this with the patient to facilitate shared decision-making. This is how we are working towards personalised medicine.” Willems thinks it’s very important to adopt an individualised approach. “Musculoskeletal symptoms tend to be chronic. It’s rarely a matter of life and death, but it is about quality of life. The patient decides what quality of life means to them. That’s why it’s so important to properly inform and support patients. This also increases patients’ understanding of their condition and their self-reliance”.
Biomedical innovation
In addition to innovating healthcare processes, Willems is working on biomedical innovations. “As the population ages, we will see a lot more musculoskeletal deformities in ageing patients, like degenerative scoliosis and vertebral collapses due to postmenopausal osteoporosis. It’s very important to find surgical techniques for weakened bones. In the PoSTuRE project, we are working together with partners like Eindhoven University of Technology and Royal DSM to develop a new surgical procedure for scoliosis, a condition in which the spine curves to the side. In this procedure, the metal screws that are used in scoliosis surgery are partially replaced by ultra-strong woven polyethylene cables developed by DSM. Loose screws can be prevented by winding these cables around the bone instead. The goal is to drastically reduce the number of complications and repeated surgeries”.
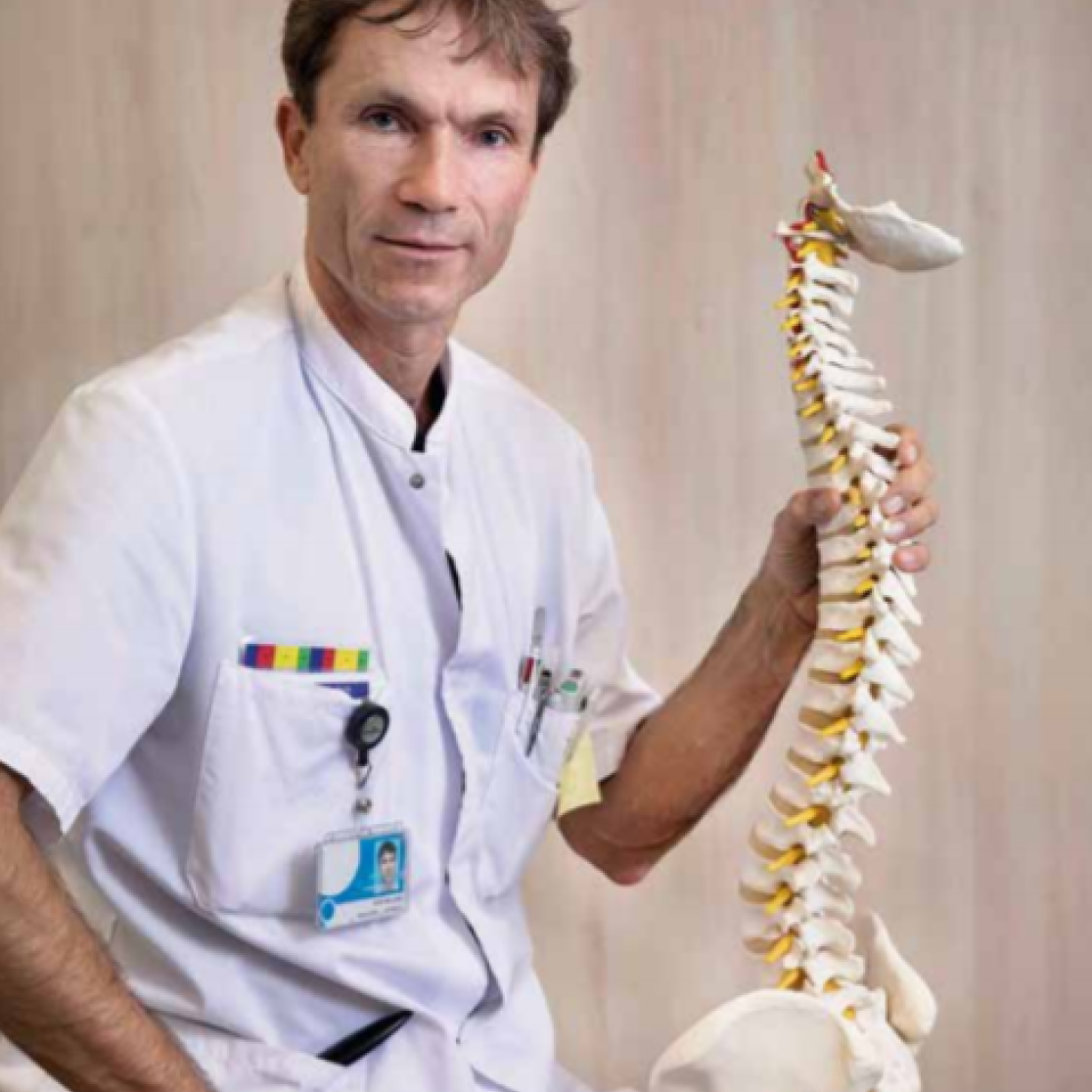
Paul Willems, PhD.
Professor of Integrated Spinal Care
Working together
They both focus on musculoskeletal conditions and they both just became professors. What else do Willems and Welting have in common? “We’re both driven by curiosity”, says Welting. “We aim to have a positive impact on individual patients’ lives by connecting science and patient care.” Willems and Welting: “To achieve that, we need each other. We need to share knowledge – the hospital, the university, our scientific network, primary care providers and tech companies. You can’t specialise in everything. People finding each other is crucial for innovation and progress.”
Text: Hanneke Trines
Also read
-
Cells, pigments or food: looking through the eyes of a microscope
How do you make the tiniest cells visible? At the Microscopy CORE Lab. Kèvin Knoops leads this research platform for light and electron microscopy.
-
Gut bacterium may help maintain weight loss
Researchers at Maastricht University and Wageningen University & Research have made a promising discovery in the fight against obesity. A new clinical study shows that a specific gut bacterium may help limit weight regain after dieting.UM news
-
Collaborative Maastricht University team receives Open Science NL funding
A multidisciplinary team of UM researchers and support staff has been awarded a €250,000 grant from Open Science NL. Their project will highlight an often-overlooked part of academic research: the people who support it behind the scenes.