Kateřina Staňková and team win $50.000 to outsmart thyroid cancer
Five teams, five days, fifty thousand dollars and one mission: to optimize cancer treatment through collaboration and mathematics. Kateřina Staňková, assistant professor at the Department of Data Science and Knowledge Engineering, found herself in the middle of an adrenaline-filled week. She co-led her team through a great challenge, resulting in a seed grant to advance their strategy to combat thyroid cancer. “People were telling me: it's the most intense thing you will ever do.”
Tension ran high at the Moffitt Cancer Center in Florida early November. A diverse group of mathematicians, biologists, doctors and computer scientists gathered for a workshop aimed at tangibly advancing cancer treatments. The catch? They had just five days to do it. The best team wins a grant to continue working on their plans. "If you hear the word 'workshop', this is not what you imagine.” Staňková is visibly excited when she talks about the experience. “You basically live with your team for a week. Even when you step outside for a break, you go together. We never stopped discussing the project."
Sleepless nights for a cause
Of course, this type of herculean effort (“I did not sleep much. The first night was the best - I think I slept for about four hours?”) is not without purpose. Staňková and her group spent five days drafting the first-ever mathematical models that describe thyroid cancer. The team included a physician, Dr. Christine Chung (Chair of the Department of Head and Neck-Endocrine Oncology at Moffitt), who works with thyroid cancer patients. She supplied her peers with patient data needed to build and validate the models, and kept them going by sharing her experiences and desire to help her patients. “She at times sees people dying. If you look at some of the patient data, it can be depressing”, Staňková says.
Advanced metastatic thyroid cancer is a so-called orphan disease: it is a rare condition, which means there is little incentive to develop new treatments. The drugs currently used to treat the disease have severe side effects and only 56% of patients survive for more than five years after diagnosis.
Smarter strategies against cancer
The workshop focused on adaptive therapy, which aims to make optimal use of existing cancer drugs. Doctors currently tend to attack cancer with the highest possible drug dose. Their goal is to kill as many cancer cells as they can, and to do it fast. While intuitive, this approach results in two problems:
- The drugs are toxic not just to the tumor, but also to the patient. This is especially true for the aggressive drugs used to treat thyroid cancer
- The higher the drug dose, the quicker a tumor develops resistance
Adaptive therapy instead employs mathematical models to help doctors decide the best course of action. “We need to play it smarter”, Staňková says. Often, patients benefit from a lower drug dose applied at shorter intervals and with breaks in between. Alternating different drugs or treatments is likely to help too. The tumor develops resistance at a slower rate, remains treatable and the side effects become less severe.
The models used for adaptive therapy integrate clinical data to predict the tumor’s response to treatment. As such, the models inform doctors on how to approach the tumor. Integrating clinical data also allows the personalisation of adaptive therapy, so it reduces drug use and improves both the quality and duration of a patient’s life.
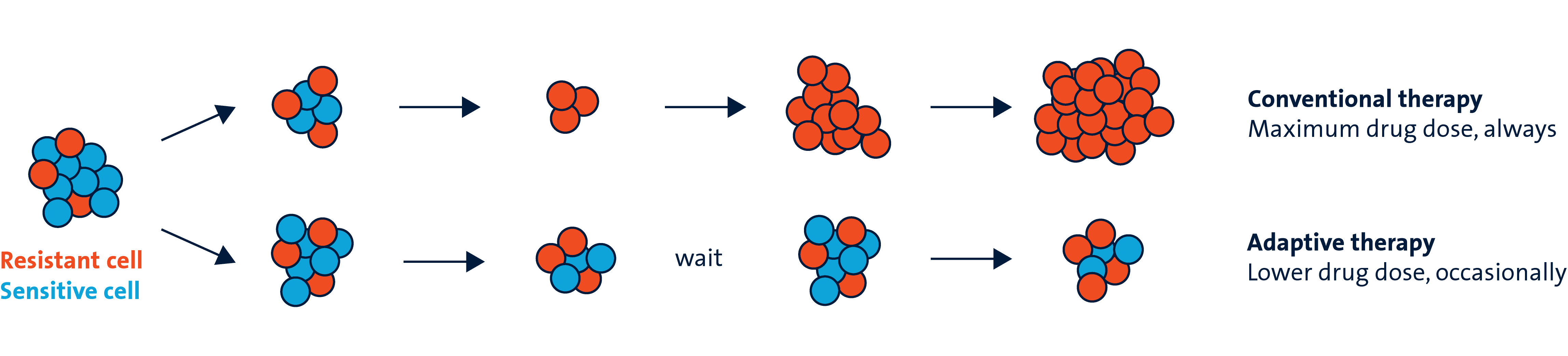
Tumors consist of different types of cells. Some cells resist treatment, while sensitive cells do not. Those cells die off in response to drugs, leaving drug-resistant cancer cells that continue to multiply. If the drug dose is too high, the tumor quickly becomes fully resistant and treatment fails. Adaptive therapy uses a lower drug dose for shorter periods of time. Treatments are paused before all sensitive cells die, as mathematical models show how maintaining some sensitive cells helps suppress the resistant cells.
We need to play it smarter.
Kateřina Staňková
Mimicking cancer mathematically
Adaptive therapy can only be a success if the mathematical models accurately describe the cancer. This was Staňková’s responsibility as the group’s lead mathematician. While the team’s diverse backgrounds were a challenge initially, they quickly proved their worth. “One of our members specialized in generating virtual patient data. I thought to myself, how are we going to use this? But then, the physician explained that we can't really prove our models, because we don't have enough data. Well, that could be the answer!" And indeed, it was: the team ended up supplementing real patient data with virtual patient data to strengthen their models.
During the fast-paced workshop, she and her team used data from about 70 patients to replicate the behavior of thyroid cancer during treatment.
Diversity in action
Staňková insists that this type of interaction is critical to the success of the project. "Someone who is not an expert would go up to the team guru and say: 'Are you sure this makes sense? I don't think it does.' The guru would reply: 'Oh, you're right, I did it completely wrong!' These kind of moments never happen if the same type of people work on the same type of problem", she explains. “The idea that you have this multidisciplinary, very diverse team, that you put people together and make them resolve something – it’s really great. You have mathematicians, biologists, cancer researchers, senior and junior scientists all sitting with a clinician, and they just work to come up with a solution.”
Seed money
By winning the challenge, Staňková and her colleagues received a seed grant of $50.000. The grant will allow trial investigations of some of the team’s more promising ideas. The money goes towards gathering more data. It will also allow the group to initiate experiments that should lay the foundations to test new types of therapy for thyroid cancer. “We are currently deciding on our next exciting steps”, Staňková says.

One thing is certain: the project was and remains a team effort. "People talk a lot about the importance of diversity. But here, I really saw it in action. I'm very happy that we won, of course, but I would have been happy with the experience either way."
The winning team
Co-leaders:
- Kateřina Staňková (Maastricht University)
- Joel Brown (Moffitt Cancer Center, MCC)
- Christine Chung (MCC)
- Christina Richards (University of South Florida)
Other team members:
- Arig Ibrahim-Hashim (MCC)
- Jeffrey West (MCC)
- Mariyah Pressley (MCC)
- Chandler Gatenbee (MCC)
- Audrey Freischel (MCC)
- Emma Carricksmith (University of Oxford)
- Matthew Wicker (University of Oxford)
- Minah Dinh (University of Washington)
- Gustavo DeLeon (Mayo Clinic)
- David Lewis (University of South Florida)
- Holly Swain-Ewald (University of Louisville)
The 8th Integrated Mathematical Oncology (IMO) workshop on Evolutionary Therapy was hosted by Alexander (Sandy) Anderson, Chair of IMO, and by Moffitt’s Physical Sciences and Oncology Center.
Go to the Department of Data Science and Knowledge Engineering website
Read article: Improving cancer patient outcomes via evolutionary game theory
Also read
-
Faculty of Science and Engineering celebrates the Weekend of Science
On 01 October, the Faculty of Science and Engineering opened its doors to host 'Weekend van de Wetenschap' (English: Weekend of Science).
-
UM scientists search for solutions to poverty and debt
Scientists from the Brightlands Institute for Smart Society (BISS) at Maastricht University are helping to find solutions to poverty and debt.
-
When you are in the middle of it, you don't just quit
Simon Schick (27) a PhD Candidate at Aachen-Maastricht Institute for Biobased Materials (AMIBM). He lives together with his fiancé in Dusseldorf. Simon is currently working on the Marie Sklodowska-Curie BioBased Value Circle Project.