Why the more we tackle ageing, the more it matters
The 20th century was, in many ways, a golden age for human health. Across the world, life expectancy rose dramatically, for example from 42.7 to 73.4 in Europe and from 49.3 to 76.8 in the USA. These improvements were driven by remarkable progress both in medical science and the economic growth needed to take advantage of these scientific advances.
I think it will be clear to most people that this increase was a good thing, but as economists we are not satisfied unless we can put a number on exactly how good… A common approach here is to try to work out how much of some other good a person would be willing to give up for a small decrease in their probability of dying. This sounds like quite a morbid question, but we actually make trade-offs like this all the time. This includes relatively small decisions like whether to drive within the speed limit, wear a bicycle helmet, smoke a cigarette or install a carbon monoxide detector; but also more major ones like whether to accept a dangerous job, or to pay a premium to live in a safer/cleaner neighbourhood. In these examples we are implicitly trading off a shorter life expectancy for something else that we value. We can use the information in these decisions to see how much people really value longevity in comparison to the other things we also want.
If we value the historical gains in longevity monetary terms, using the willingness to pay approach, we find them to be absolutely huge. In an influential 2006 paper, Murphy and Topel showed that improvements in US life expectancy across the 20th century were roughly equivalent to every person’s income being around 40% higher every year for the whole century! In a paper together with Andrew Scott, Martin Ellisson and David Sinclair, we apply this approach to a range of countries and find similarly massive numbers. For example, taking into account improvements in both health and life expectancy, we estimate the improvements in longevity in the Netherlands from 2000-2009 to be worth €30.100 per person per year.
When I first started working in this area, I was really struck by how powerful and valuable these changes are. Once you think about it, I think these magnitudes also make a lot of intuitive sense. In many of our lives, the most binding constraint we face is time. Whatever it is we find valuable and meaningful, we could have or do more of it if our lives were longer. In that context, it makes sense that we would be willing to pay huge amounts for longer lives.
1 Data from Our World in Data and World Bank Development Indicators.
A 21st century slowdown
However, in the 21st century, the longevity story is not quite so astounding as in the 20th. While European life expectancy increase by an average of 3.4 years per decade from 1900-2000, since then the increase has fallen to only 2 years per decade. For the United States, this is even more striking which saw increases of 2.93 years per decade in the 20th century, but only 0.73 since 2000. In fact, US life expectancy is actually lower now than it was in 2014. Similarly, if we look at healthy life expectancy, a measure which adjusts for quality of life, we see a slowdown in progress in Europe and a reversal in the US. At the same time, around the world, countries are spending an increasing share of their income on healthcare. So we are spending more on health and getting less for it in terms of health gains. Why is this?
Our answer, developed across a series of papers, is that we are living through a fundamental epidemiological transition – a shift in the dominant causes of death across a population – where the disease burden has shifted away from the conditions that medicine conquered in the 20th century and toward a new dominant force: ageing.
The Increasing Dominance of Ageing
The increasing dominance of ageing is already apparent from just the mortality data. In a 2025 paper with Andrew Scott, we used a statistical approach to explain and predict how the mortality-age relationship has evolved over the last 100 years. Here we find that the key driver of life expectancy is now late-life mortality and that this dominance is likely to continue to increase.
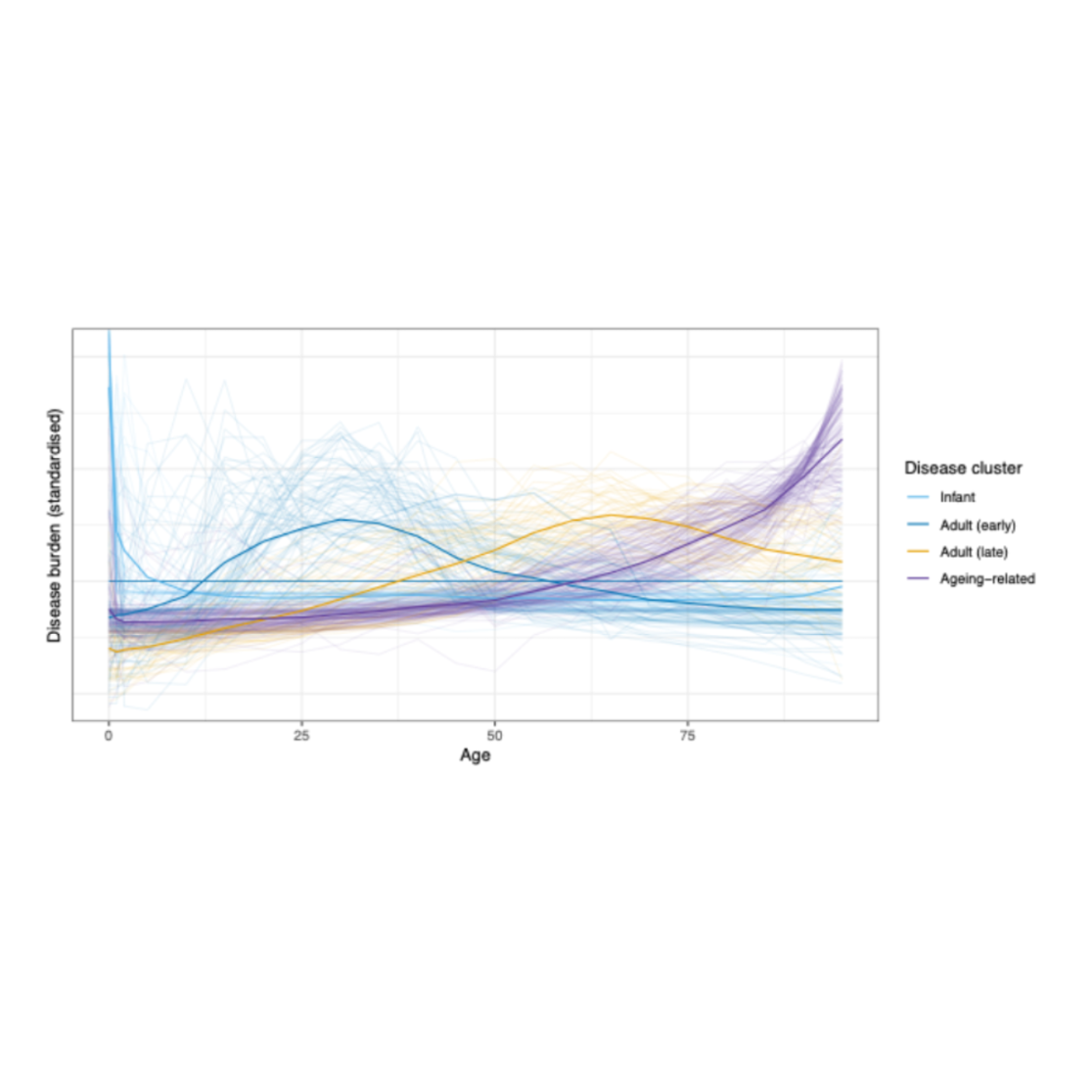
In more recent work, we look at this in a more holistic way, taking into account health and using the willingness to pay approach discussed above. We use a statistical clustering method applied to Global Burden of Disease data to group diseases not by their biology but by when in the life course they strike hardest. This produces four natural clusters: infant diseases, early adult diseases, late adult diseases, and the critical fourth group of ageing-related diseases. As shown in the chart below, ageing-related diseases are characterised by a burden that rises continuously with age.
Before thinking about this in monetary terms, we can look at the current burden of each of these disease categories purely in terms of health and mortality. To do this, we use the concept of Disability Adjusted Life Years (DALYs) – a way to estimate how much healthy life is lost because of diseases and injuries. The DALY cost of a given disease adds together Years of Life Lost (years lost when people die earlier than expected) and Years Lived with Disability (years lived with illness or disability that reduce health). The Table below shows how the current burden of all diseases are spread across our disease categories, both globally and separately for each group of countries by income.
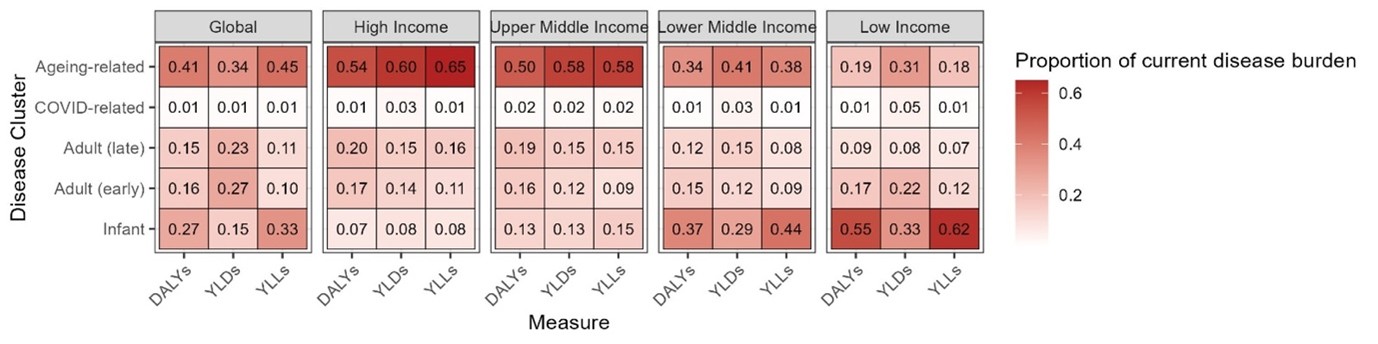
As the Table clearly shows, globally and in high and upper middle income regions, ageing-related diseases are by far the biggest portion of the total disease burden,
If we do put a monetary value on reducing the prevalence of diseases in each of the four clusters we, perhaps unsurprisingly as we are focussing on a developed country, find that by far the biggest value is in tackling ageing-related disease. However, we find some genuinely surprising results when we look at how the value of tackling each type of disease changes the more we do it. Here we find that tackling ageing-related diseases has the unique property of increasing returns to scale.
A Virtuous Circle: the Increasing Returns to Tackling Ageing
Just looking at the current burden of different disease clusters is useful, but in reality we are not just interested in one-off interventions. As we make progress, the relative value of different options is likely to change. To get at this, we calculate the social willingness to pay for successive reductions in each disease cluster, a remarkable asymmetry emerges, which can be seen in the chart below.
For infant, early adult, and late adult diseases, the value of further reductions is roughly constant or mildly diminishing. It is always good to reduce these diseases, but each additional improvement is worth around the same as the previous one. Ageing-related diseases are completely different. The more progress we make in reducing them, the more valuable each additional step becomes. We show this analytically and numerically: there are strongly increasing returns to tackling ageing-related disease.
The mechanism works through two channels. The first is purely about mortality and life expectancy. Reductions in ageing-related mortality are especially powerful because they strike at ages where both the probability of still being alive and remaining life expectancy are highest relative to the size of the mortality impact. Because ageing-related diseases are defined by an upward-sloping mortality curve, progress always opens a new window of opportunity where further reductions have large proportional effects on both survival and remaining life expectancy. This creates a self-reinforcing dynamic.
The second channel operates through a complementarity between mortality and morbidity (ill-health). Ageing-related diseases are unique in that they damage both health and survival at the same point in the life cycle. Reducing them therefore generates improvements that compound: better health at older ages makes people more willing to spend, shifting consumption toward later life, which in turn makes longer survival even more valuable.
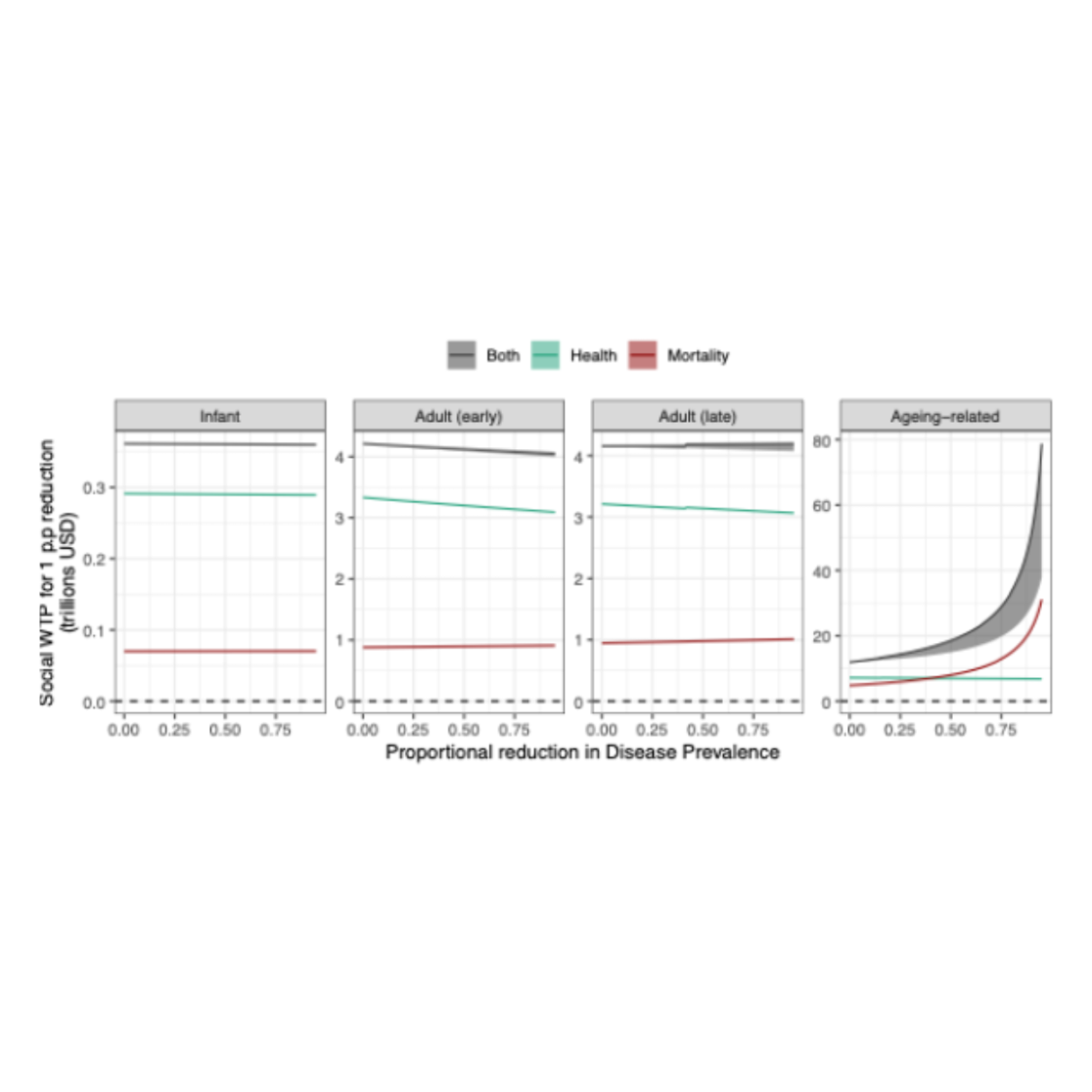
Our analysis accounts for the fact that living longer means stretching income over more years. Even including this cost, the increasing returns remain powerful. What is more, we have not factored in that healthier ageing may allow people to work longer and earn more. Including these labour market effects would make the case even stronger.
One might ask: if increasing returns to tackling ageing are so, why has this only become a dominant policy concern recently? The answer here is that until relatively recently there were still very large gains to conquering early-life and midlife diseases. However as these gains have been made, it does not become any more valuable to make further progress. In contrast, the increasing returns to tackling ageing we identify suggest that this will only become a more and more pressing concern the more progress we make. The 20th century was characterised by an epidemiological transition in which populations shifted from deaths mainly caused by infectious diseases and malnutrition to deaths mainly caused by chronic, non-communicable diseases like heart disease and cancer. Today, we are at the start of a new transition as we enter a world where the central health challenge, and the central health opportunity, is ageing.
Looking Ahead: Healthy Ageing and the Labour Market
The analysis so far has focused on welfare: how much people value longer, healthier lives in their own right. But the economic consequences of achieving healthy longevity extend further, and this is where my current research agenda is heading, supported by a VENI grant that I was recently awarded.
The central question is: as people live longer, what happens to work, productivity, and retirement? European policymakers are very concerned about this question, with fears that ageing populations and shrinking working-age cohorts will strain pension systems and labour markets across the continent. The extent to which this will manifest depends crucially on whether our longer lives are also healthier lives, and in what sense they are healthier. This is both a measurement challenge, as it is not clear what aspects of health are most relevant for people’s ability and inclination to work, and also a theoretical challenge as we need to consider how changes in health and longevity affect both the system as a whole and differences across individuals.
The increasing returns result we have established for health and welfare may well have a parallel in the labour market: the better we age, the more productive and engaged older workers can be, compounding the gains from further improvements in healthy longevity. Establishing whether that virtuous circle operates in the labour market is, I think, one of the most important questions in the economics of ageing for the decade ahead.
The story of the 20th century was one of remarkable progress, but the 21st century presents a different challenge, and a different opportunity. As the gains from conquering early-life diseases have been banked, the frontier of health has moved to ageing. Our research suggests that the more progress we make there, the more valuable each further step becomes. Understanding and acting on this virtuous circle may be the defining health challenge of the decades ahead.

Want to know more?
To explore this theme further, Julian has shared his research across multiple platforms. He recently joined the CEPR podcast to discuss the economics of longevity, and wrote a VoxDev blog exploring how language modelling can help analyse aspirations among Rohingya refugees.
In our new SBE Podcast episode, he reflects on the economic and political challenges of ageing societies, the role of health in shaping labour decisions, and why new approaches to measuring health may be needed. Listen to the full conversation or watch it on YouTube.
Also read
-
The beating heart of ROA for 38 years: Margo looks back
Margo Romans looks back on 38 years at ROA: from the institute’s youngest employee to one of its indispensable pillars. She witnessed ROA grow from a small team into an internationally recognised research institute, while collaboration, commitment and the sharing of knowledge always remained.
-
From pioneering phase to established institute: former directors Andries de Grip and Rolf van der Velden look back
Former directors Andries and Rolf reflect on ROA’s growth from a small team into an influential institute. Its success was driven by a strong focus on relevant research, data and collaboration. Despite the institute’s growth, its culture, team spirit and strong intellectual direction remain.
-
Problem-Based Learning meets AI in the classroom
Marc Becker is investigating how the success of AI depends on its social skills, given that AI is increasingly beginning to function as our colleagues, managers, leaders, and even teachers. Among other things, his research explores how AI can support students’ learning process.