Captain Space-Heart
MERLN’s Lorenzo Moroni coordinates a European consortium that develops a technology to create heart ventricles in space using magnetic and acoustic levitation. The subsequent research on the International Space Station will have significant benefits for the humble inhabitants of Earth.
Why in space, you may wonder. Because everything’s more awesome in space! Also, in keeping with NASA’s and ESA’s ambitions to have permanently inhabited basecamps on the moon, first aid becomes more tricky. “The field of biofabrication, where we try to engineer tissues by depositing cells and biomaterials in an automated fashion for therapeutic purposes, is already quite advanced and those space agencies are open to supporting research that promises to help them,” Moroni explains.
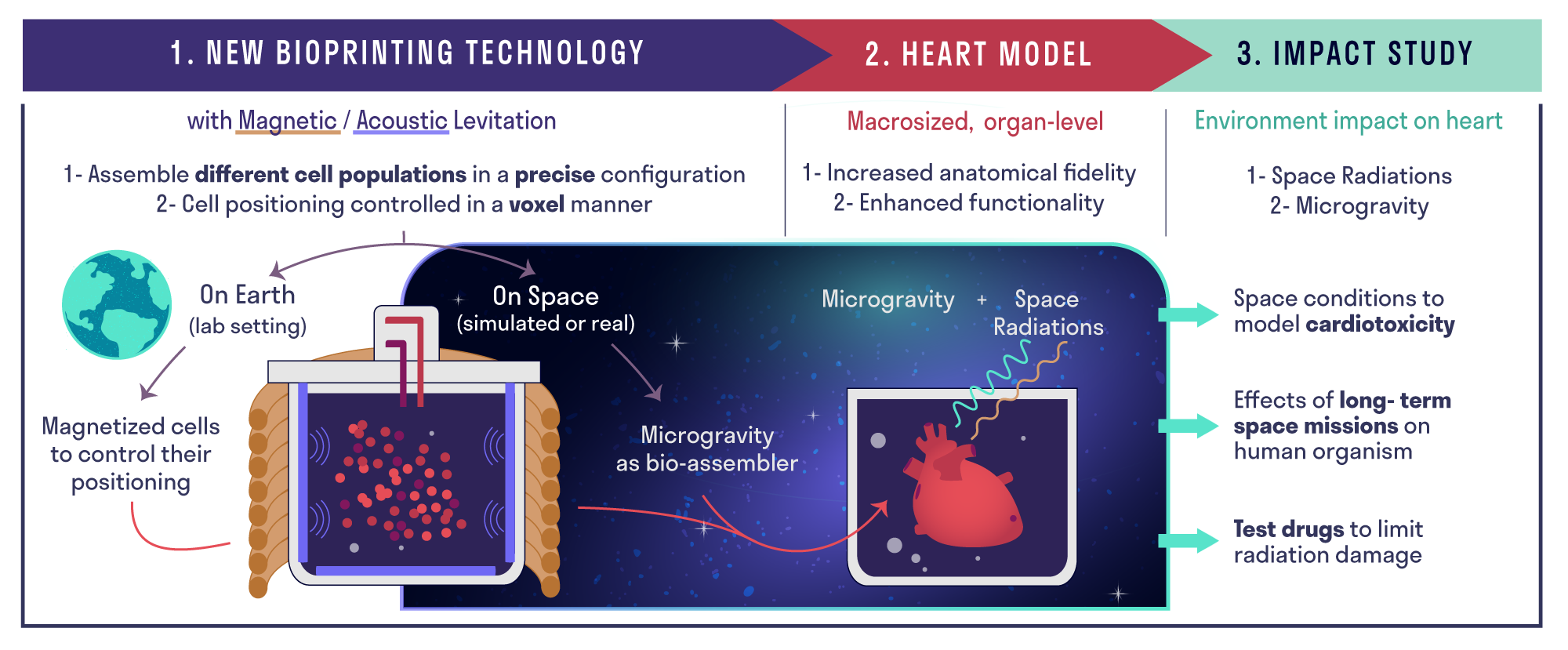
To the Professor of Biofabrication for Regenerative Medicine and his team, space has a very pragmatic advantage: things levitate easily. “We will make biological substitutes similar to cardiac ventricles using a mixture of magnetic and acoustic levitation. Both methods have been trialled on their own – magnetic levitation has been around for 50 years – but the combination is novel. This allows us to move cells in a volume. The result is a closer mimicry of the architecture of human tissue than something printed in layers would be.”
An ageing heart among the stars
Cardiac ventricles are the chambers of the heart that pump blood to the rest of the body. Irregular contractions of these ventricles are the most common cause of cardiac arrest. “If you take a human tissue biopsy, you see cells and proteins. The proteins typically have an organisation, sort of like a scaffolding system, specific to the type of tissue. We use a polymer-based gel to mimic that scaffolding structure. The gels are designed in such a way that they can then be degraded by the cells and replaced with the natural protein structure formed by the cells.”
In this gel, Moroni and his team will place the cells. “We use stem cells, which have the potential to turn into any specialised cell; in this case, cardiac cells for blood vessels, which supply the tissue with nutrients, and cardiac-associated fibroblasts, which keep the cardiomyocytes, i.e. muscle cells, in place.” The result is a living tissue, which will contract, i.e. beat, the way a ventricle would.
Space-heart: excellent! Why not? At the same time: why? “In space, there’s little to no gravity and, more importantly, there is little protection from cosmic radiation, which causes DNA damage in cells. This means tissues age a lot more quickly there. We can use the ventricle to study cardiac physiology. In particular, we can look at the ageing process and we will also study the effects of novel drugs to ameliorate the effects of ageing. The potential impact on cardiac health is enormous.”
Space exploration boosting pharmaceutical advancements
Not only are these tissues easier to synthesise in space – thus at least the hypothesis – since the machines to create the magnetic and acoustic fields for levitation can be a lot smaller: after all, there is a lot less gravity to counteract. It is also more practical to transport the respective machines there than the quasi-alive tissue. “Obviously, the space agencies also see the potential in the long run for biofabrication to be used in medical emergencies among space travellers.”
Moroni praises space exploration as a booster for technology as a whole. “I also see potential for studying other tissues, like bones and muscles for example. You can see astronauts struggling to walk when they come back because of muscle atrophy and being more prone to bone fractures and osteoporosis in the long run.” Conventional before-and-after tests on astronauts are difficult and problematic for obvious reasons, so the advantages of studying biofabricated tissues are clear (also to the unbiopsied astronauts).
Launch in less than 5 years
Rather than heart-textured pie in the sky, there are concrete plans. With a €4 million grant from the Horizon Europe 2027 programme of the European Community (under the Pathfinder Open scheme), Moroni’s project will bring the new bioprinting technologies to create models for studying cardiac physiology to the International Space Station (ISS).
“The last years made collaboration more difficult, so that threw off the planning, but we should have everything set up in the ISS by summer 2027.” Moroni has been in talks with the agencies for more than four years now and has also assembled an interdisciplinary European consortium of experts on radiation, microbiology, microgravity, pharmacology, the physiology of astronauts, as well as space engineering and logistics.
Moroni is used to interdisciplinary collaboration, which he says is innate to his field of research. His career in science has always been motivated by a desire to help people. Growing up in Milan, he was inspired by his uncle, a cardiothoracic surgeon. However, somewhat serendipitously, he failed the entrance exam to become a physician and studied biomedical engineering instead, combining his passion for engineering with his interest in medicine. This allowed him to enter the relatively new field of regenerative medicine.
Profoundly interdisciplinary
While Moroni has studied cardiac biology for more than 20 years, he has never witnessed someone die of a heart attack. It is in this spirit of humble inquisitiveness that he approaches interdisciplinary collaboration. “It is just too complex – of course you can’t know everything in detail. Modern science is about working in teams on a daily basis instead of everyone remaining in their own environment and only meeting once a year at a conference.”
While acknowledging the tremendous challenge to communicate effectively across disciplinary frameworks – and personalities, Moroni thinks the scientific progress easily justifies the effort. “As coordinator, I have to keep the bigger picture in mind and remind people to get behind the common goal, to come up with ways of helping people. Even though we won’t see the direct impact of our work like a physician would, it’s still great to contribute, to be a link in the chain from research and development all the way to curing patients.”
By: Florian Raith
Also read
-
The University Fund Limburg's new Annual Fund Campaign is live!
Every year during the holiday season, the UM community comes together to uphold a special tradition: supporting projects that contribute to a healthier, fairer and more sustainable society. Will you join us?Featured,Researchers andStudents
-
SBE researchers involved in NWO research on the role of the pension sector in the sustainability transition
SBE professors Lisa Brüggen and Rob Bauer are part of a national, NWO-funded initiative exploring how Dutch pension funds can accelerate the transition to a sustainable society. The €750,000 project aims to align pension investments with participants’ sustainability preferences and practical legal...Featured,Human interest,Researchers andUM news
-
Fresh air
Newly appointed professor Judith Sluimer (CARIM) talks about oxygen in heart functioning and the 'fresh air' the academic world needs.Featured,Researchers andUM news