"Het mes kan van tafel"
There is a saying in Dutch: “Met het mes op tafel” which translates to “With the knife on the table”. In the context of behaviour or negotiations it means acting tough, not giving in, showing that someone means business. “Het mes kan van tafel” translates to “the knife can be taken off the table”, which in a surgical context has a thought-provoking double meaning.
Having an impact in people's lives and on society as a whole. Being able to make a real difference. That is what Prof Klara Mosterd wants to achieve with her research into skin cancer and the clinical treatment of patients. When you consider that 1 in 5 people in the Netherlands are affected by skin cancer, it is clear that she can have a lot of impact with her work. Klara Mosterd was appointed Professor of Oncodermatology in 2022, occupying the first chair at Maastricht University in this field in the Netherlands. On 17 March 2023, she will deliver her inaugural address titled ever so intriguingly: “Het mes kan van tafel”. A symposium will also be organised on that day.
Skin cancer is currently the most common cancer diagnosis in the Netherlands and the number of cases is increasing. Therefore, conducting research on skin cancer treatment has become much more relevant to many more people. The fact that the number of diagnoses is on the rise is partly due to the ageing population: skin cancer is a disease common in the elderly. In addition, how we conduct ourselves in regard to sun safety plays a role. Klara Mosterd: "You have to remember that skin cancer is some 30 to 40 years 'behind'. The patients we see now are mostly people who went out in the sun decades ago – much more so than the generation before them. We are really dealing with a peak now, a catch-up effect of all those years of sun worship."

Klara Mosterd is a skin cancer expert and dermatologist working at the MUMC+ Comprehensive Cancer Center. She is part of the multidisciplinary head and neck team and responsible for the work-up and treatment of patients with skin cancer. Klara Mosterd is a professor in oncodermatology at Maastricht University and GROW School for Oncology & Reproduction. She is principal investigator of many clinical multicenter trials but also conducts molecular research concerning the causes of basal cell carcinomas. Her research is partially funded by the Kankeronderzoeksfonds Limburg.
The title of your speech is: “Het mes kan van tafel“ – tell us how you see that?
Mosterd: "Over the past 10 years, we have made tremendous progress in treating and diagnosing skin cancer without surgery. Compared to 30 years ago, when just about everything was cut away, there are now more and more non-invasive treatments available. Of these, we now know much better what we are doing and whether what we are doing is right. We have made great strides: in diagnostics thanks to the OCT scanner, and in treatment thanks to comparative studies on the effectiveness of creams and ointments for treating skin cancer and the advent of immunotherapy. Firstly, the OCT scanner: Maastricht UMC+ is the first hospital in the Netherlands where we started working with these new diagnostics in skin cancer. We have conducted large-scale research into the reliability and effectiveness of this scanning method and are achieving very good results with it. In the field of non-surgical treatments, there have also been many developments in recent decades, such as the use of creams and ointments, with which especially the smaller tumours – the basal cell carcinomas – can often be treated effectively. Secondly – specifically for the more aggressive form of skin cancer, melanomas, which I do not deal with as often – the discovery of immunotherapy is also a development that means a lot this field. With this, the chances of survival and sometimes even complete cure have increased many times over."
"Besides this very literal approach of “Het mes kan van tafel”, I also mean it figuratively. It is incredibly important that we collaborate in healthcare. Really collaborate, not oppose each other. That applies both in our organisation and in regional and national collaborations. Outside Maastricht, only a few centres used to do skin cancer research. Now this research is conducted in many places and I think that's great. Collaborating with each other in studies and research instead of competing – certainly in a small country like ours – that's where the future lies. It also lies in cooperation in the field of treatment. It should make no difference to a patient's life expectancy in which location he or she starts treatment. The increased number of treatment options makes it essential that we, as skin cancer specialists, discuss these options with each other. Multidisciplinary consultation structures, in which different specialists discuss a treatment choice and the case can be examined from all sides, have become increasingly important in recent years. Achieving solid unambiguous guidelines together while also leaving room for individual consideration. For example, an operation may give a better chance of cure, while surgery may not be desirable for the quality of care nor the preservation of the patient's function."
Interview continues below the picture
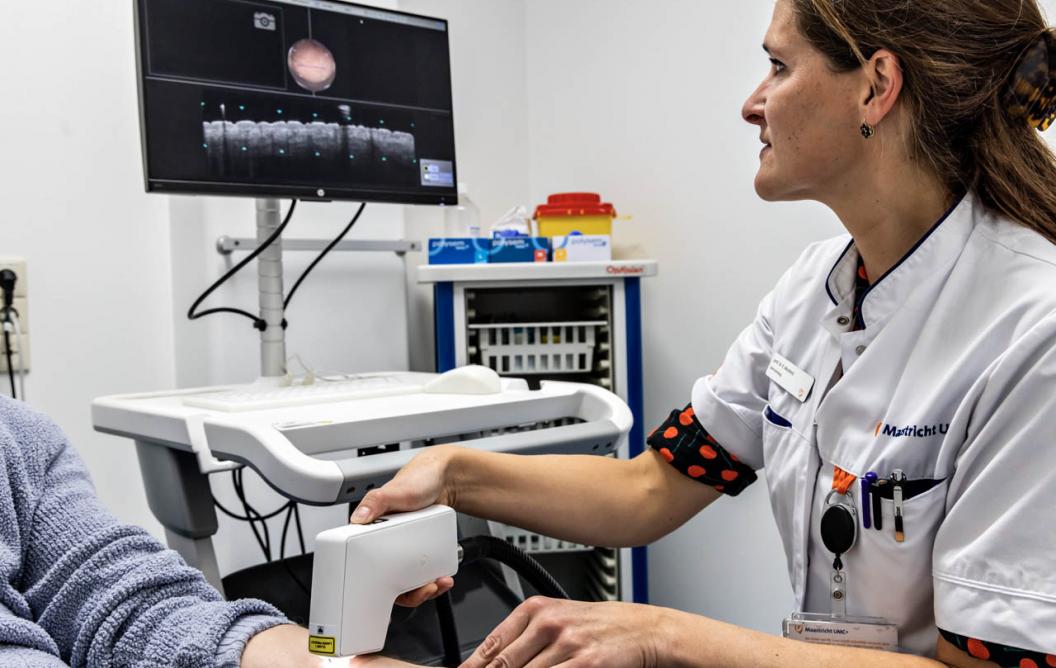
OCT stands for optical coherence tomography. The OCT scanner uses infrared waves to make an image of the skin. On this basis, it can be determined (with 65 percent certainty) whether it is a basal cell carcinoma or benign.
What are the major advantages of these new non-invasive treatment options?
"It is preferable for patients not to have to undergo surgery, especially if they have tumours in several places. Further to that, it can also be very useful to give this type of treatment if people cannot come to hospital or if it causes a lot of hassle for the patient. Especially for older people with multiple areas that need to be treated, it makes sense to try an ointment first. After all, if we can remove 80 per cent of tumours with this approach, only 20 per cent need to be treated surgically. Surgery may still be the most effective, but skin cancer is most often on the face and surgery always leaves a scar. Treatment with an ointment or a salve gives a better result cosmetically."
A lot of positive things are happening in your field and there is already much less surgery. Do you think the knife can really be taken off the table altogether?
"I haven’t ruled it out. It won't be in the next two years, but in 10 years it could be a reality. As we continue to refine our protocols and treatment plans, gain more knowledge on which treatment works for which type of cancer and we combine treatments, you can eventually get to 100 per cent. That stretch is there. We haven't pulled out all the stops yet. "
Where will the focus be within your chair in the coming years?
"I have three lines of research under way and there are gains to be made in all these areas. The first line of research concerns cost-effectiveness studies. These are very important for keeping healthcare affordable. Together with other centres, we do research into treatments that are now 'standard of care' but for which it is not yet clear whether the treatment should take place and which is the best. We hope to soon start a large-scale study into whether someone really needs to be treated for a certain preliminary stage of skin cancer. This is now carried out to be on the safe side, but the numbers involved are really incredibly large, as about 50% of over-45s are walking around with such a condition."
"The second line of research is about non-invasive diagnostics and, in particular, how do we roll out the possibilities we have found in our OCT scanner research throughout the Netherlands. We are now the only centre in the Netherlands where the dermatology department has such a device. The national implementation of the OCT scanner still involves an awful lot. Who will work with it? Dermatologists? Or could it also be analysts or nurses? What does the learning curve look like? When do you really dare to replace a biopsy with this technique? We are currently setting up this implementation from here in Maastricht. "
"Finally, the third line of research concerns rare forms of skin cancer, in particular basal cell naevus syndrome. Patients with this condition sometimes develop hundreds to thousands of basal cell carcinomas due to a genetic defect. This obviously has a huge impact on their lives. MUMC+ is a centre of expertise in this field. Thanks to a new guideline we created – which has also been recognised at European level – the care for these patients is now, fortunately, much better worldwide. What is further interesting is that although the condition they have is rare, basal cell carcinomas are actually incredibly common. By learning more about the very rare condition, we also learn about the non-rare cases and can ultimately treat that large group better as well."
How does society and the individual patient benefit from your scientific input?
"1 in 5 people get skin cancer, so any improvement in care that takes place has an effect for a very large part of the population in the Netherlands. The 4 others who don't get it also benefit. The cost of healthcare is huge so if we make sure that care is organised more efficiently and patients get the right treatment and are not over-treated, more will be left in the end."
Where do you hope to be in five years' time?
"I hope that OCT will then be used in a very large part of the Netherlands in the diagnosis of skin cancer and that by then the use of artificial intelligence can help us make diagnoses with even more certainty and more quickly as well. I hope that, by then, we will see a large proportion of patients with low-complex skin cancer or its precursors less frequently in hospital. That those patients will simply be treated at home or maybe even no longer need treatment. Also, that the many skin cancer check-ups can be phased out by then, reducing the huge pressure of skin cancer patients that we still experience today and allowing more space to treat the complex skin cancer patient."
"I hope that in five years, a large proportion of patients with low-complexity skin cancer will be treated simply at home."
Follow Klara Mosterd's inauguration here.